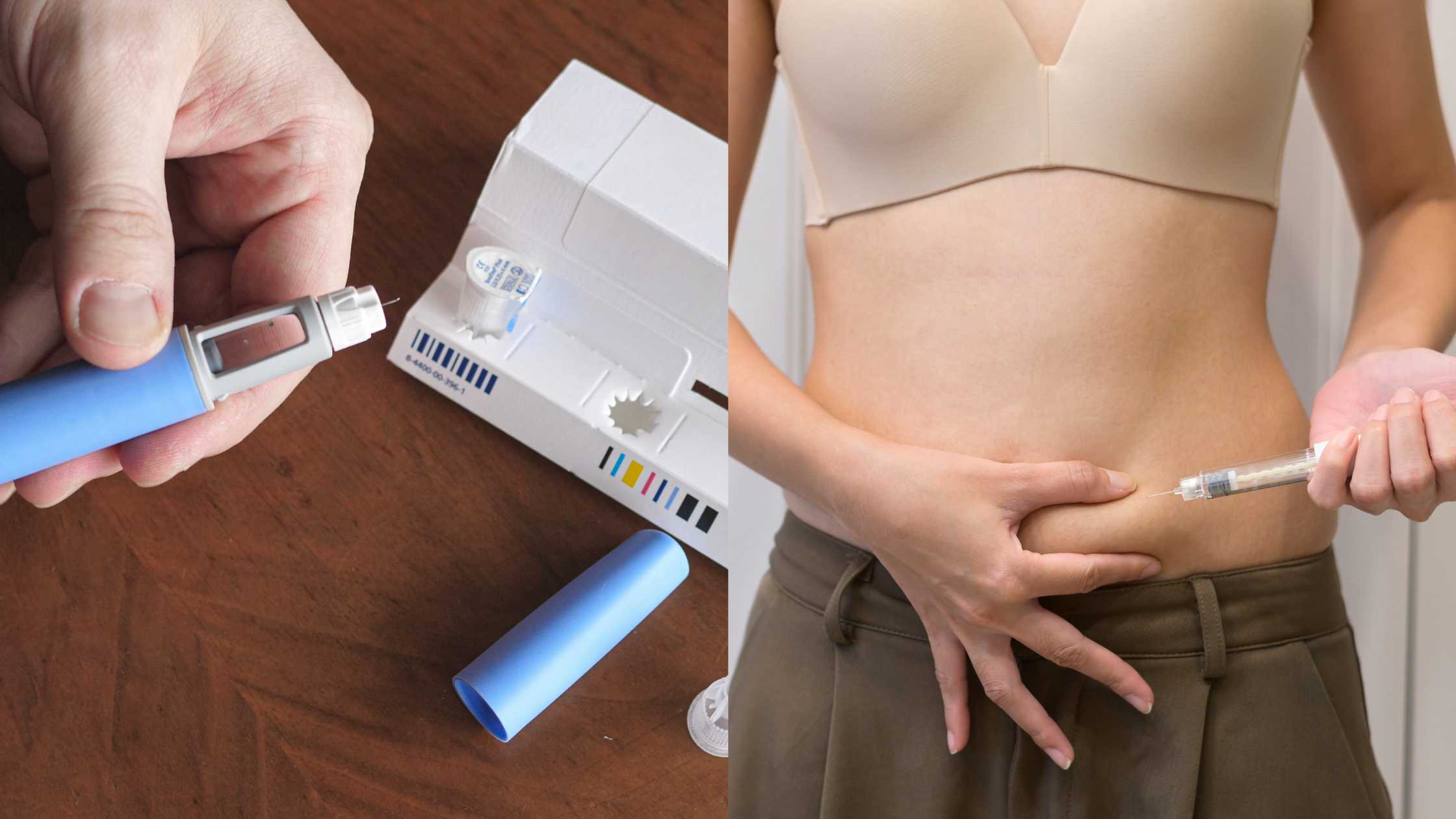
Key Takeaways
- GLP-1s and liposuction play very different roles in body transformation and can actually complement one another when paired. GLP-1s fuel systemic, slow weight loss while liposuction contours specific fat pockets.
- Think of liposuction as a final spark to your existing results. This is only after hitting or approaching your goal weight and keeping it consistent for a few months, where contouring is most predictably achieved.
- Liposuction targets stubborn subcutaneous fat, the type present in the abdomen, flanks, thighs, arms, and chin. It doesn’t reduce visceral fat or consistently tighten skin laxity.
- For optimal long-term results, coordinate GLP-1 treatment with sustained lifestyle habits, mental health support, and when necessary, supplemental treatments like skin tightening.
- Evaluate risks, recovery and medical suitability prior to combining treatments. Follow a staged timeline that permits weight stabilization, surgical planning and precise post-op care.
- Try non-surgical contouring for subtle touch ups if you want less downtime. Weigh advantages and disadvantages with an expert clinician to determine the safest, most effective solution for your objectives.
Refine Ozempic Results with Liposuction is a surgical option that targets stubborn fat post-semiglutide weight loss. Liposuction helps shape and contour the body by eliminating targeted fat pockets.
Candidates typically have stable weight and reasonable expectations. Recovery differs by area addressed, but generally consists of mild swelling and a few weeks of decreased activity.
What you need to know about timing, risks, and cost, plus how to pair procedures for safer, lasting results.
Two Paths
Pharmacological or surgical approaches represent two very different strategies for fat and figure loss. One shifts metabolism and appetite with GLP-1 receptor agonists over time. The other uses liposuction to remove fat in targeted areas instantly.
Both have defined functions, boundaries, expenses, and recuperation requirements, and for a lot of us, optimal output results from mixing them.
The Mechanism
GLP-1 drugs hit brain and gut receptors to curb appetite, delay gastric emptying, and boost insulin sensitivity. Such transformations yield consistent, sometimes months-long weight loss, and they enhance markers such as blood glucose and blood pressure.
Liposuction involves small incisions and cannulas to physically break up and vacuum fat cells from beneath the skin. The impact is immediate in volume excised, although edema and tissue reconfiguration make the final contour emerge over weeks to months.
GLP-1s shift systemic energy balance and deplete total body fat stores and some visceral and subcutaneous fat loss, whereas liposuction only eliminates subcutaneous fat and does not significantly impact visceral fat or metabolic risk.
Two roads in one – how a metabolic tool can reduce total fat as surgery sculpts form where diet, exercise, and pharmaceuticals leave lingering bulges.
The Target
GLP-1 therapy targets total body weight and fat percentage, not a specific area of the body. It’s helpful when your target is improved metabolic health and long-term weight management, which is significant for individuals with type 2 diabetes or metabolic syndrome.
Liposuction targets localized, stubborn deposits that haven’t responded to lifestyle or medications. It’s a targeted sculpting wand for those who desire enhanced contours post-weight loss or without substantial weight fluctuations.
- Abdomen (upper and lower)
- Thighs (inner and outer)
- Flanks/love handles
- Arms (underarm/upper arm)
- Chin and neck
Liposuction enhances proportion and will never substitute for the systemic benefits of real weight loss.
The Purpose
GLP-1s are approved to treat weight and metabolic health with frequently ongoing doses and monthly costs that can add up. Liposuction serves cosmetic goals: to correct asymmetry, remove stubborn fat, and create smoother contours with a one-time surgical expense, followed by a recovery period of weeks and possible downtime.
For most, GLP-1s assist in achieving a more optimal weight and lipo polishes the visible result once weight is maintained. The two paths differ in speed and permanence.
Drugs produce gradual change and ongoing maintenance. Surgery produces an immediate change with healing over months and permanent removal of treated fat cells. Cost, recuperation time, and individual objectives factor into which trajectory or mix suits best.
The Synergy
The synergy of liposuction combined with GLP-1 therapy creates a concerted effort to sculpt your post-medical weight loss physique. GLP-1 meds change appetite, increase meal-induced insulin release, slow gastric emptying, and can generate 15 to 22 percent weight loss in trials. Meanwhile, liposuction removes localized fat deposits that linger after systemic weight loss. Together, they tackle metabolic drivers and aesthetic sculpting by enhancing contour and typically reducing recovery by providing better-prepped patients.
1. Stubborn Fat
A lot of patients shed massive amounts of weight with GLP-1s but retain modest, stubborn fat in areas that are poorly responsive to either diet or drugs. These are areas like the lower abdomen, love handles, inner thighs, bra rolls, and submental fat. Liposuction zones in on these pockets, with precise cannulas suctioning fat away and contouring the space.
For instance, an 18% total weight loss patient can still have a stubborn lower abdomen pooch. Eliminating that fat can cause waistlines to sit in better clothes and reduce unevenness. A simple checklist of common zones helps surgeons and patients plan: lower abdomen, flanks, medial thighs, upper arms, and submental area.
2. Body Proportions
Too fast or too much weight loss can leave lumpy contours or a “skinny fat” appearance where fullness is depleted unevenly. Liposuction brings back proportion by removing excess fat from bulges and depositing a little more where there was less or by pairing with fat grafting to add volume where desired.
Case tables showing waist-to-hip changes or hemline balance are helpful to set expectations. When you achieve a proportional shape, it maintains overall satisfaction and makes your clothes fit better, which is frequently a high priority among patients.
3. Skin Laxity
Large loss from GLP-1 therapy can unearth loose skin. Liposuction by itself does not tighten the skin and could actually exacerbate skin laxity if there is too much redundant skin. Tummy tucks, or arm or lower body lifts may be needed to excise excess skin.
Newer skin-tightening devices and regenerative approaches can assist mild cases, but a customized surgical strategy remains key. Redundant skin impacts comfort and function as well as cosmetics, so evaluation must encompass quality and elasticity of skin.
4. Final Contours
Liposuction is the icing on the cake once weight is fixed. Modern techniques allow precise sculpting to refine the final shape, but timing is key. Wait until weight and medications are steady for optimal results.
A stepwise transition plan from GLP-1 to surgery, which includes discontinuing or controlling medications, preoperative labs, and staged procedures, lowers risk. This staged approach provides enduring contour benefits and encourages long-term weight control.
5. Psychological Boost
Sharpening weaknesses tends to bolster confidence and reward virtuous cycles. Patients tell me they feel more confident after combined treatments and recorded before and after case studies can capture emotional as well as physical transformation.
Better body image often supports lifestyle changes and weight maintenance.
Ideal Candidate
The perfect candidate is someone who has reached or is close to their goal weight with GLP-1 meds like semaglutide (Ozempic) and now desires focused contouring. This is someone who used systemic therapy to reduce bulk and is now left with small, stubborn pockets that do not respond to diet, exercise, or continued medications. Most are type 2 diabetics who initiated GLP-1s for metabolic indications and discovered the bonus of shedding pounds, or those who initiated GLP-1s to shed pounds after everything else failed.
Candidates who had a high BMI or comorbid conditions and then lost significant weight, frequently 15 to 20 percent of starting weight, are common, particularly if there is loose skin or localized fat. Candidates must demonstrate weight stability for a period of time prior to surgery. Stable weight means no more than small fluctuations for 6 to 12 months, showing that metabolic changes have stabilized and that surgical reshaping will be permanent.
Being stable allows the surgeon to map out precise fat excision and minimizes the likelihood that additional weight fluctuation will impact results. Patients still losing a ton of pounds or who resume aggressive weight-loss plans soon after surgery risk patchy results. Medical fitness and grounded expectations are needed. Eliminate individuals with significant medical risks like uncontrolled diabetes, active CAD, clotting disorders, and the like, or poor wound-healing history.
Rule out individuals who anticipate lipo to be a replacement for weight loss or a repair for body-image insecurities without lifestyle adjustment. Good candidates know what liposuction can and cannot do: it removes localized fat, it does not tighten large amounts of loose skin, and it requires recovery time and follow-up care. Hands-on preparedness and dedication make things better.
Ideal candidates are self-driven, monitor weight and body fat, visit post-op appointments, and adhere to pre- and post-op directions. They have experimented with non-invasive solutions, such as diet, exercise, and persistent GLP-1 use, for stubborn fat and observe little difference. They understand combined care, which involves coordinating with their prescribing clinician to time cessation or adjustment of GLP-1s if required, optimizing nutrition and blood sugars before surgery, and planning realistic downtime.
Eligibility checklist for safe, effective combined treatment:
- Achieved or close to goal weight on GLP-1 therapy and stable for six to twelve months.
- Lost a significant amount of initial weight, typically 15 to 20 percent, or cannot spot reduce with traditional, non-invasive methods.
- Medically cleared: controlled comorbidities, no active infections, and an acceptable clotting profile.
- Understand fat removal and possible skin procedures.
- An ideal candidate would be willing to self-weigh and adhere to post-op care.
- Coordinated care plan between bariatric/medical provider and plastic surgeon.
Strategic Timing
Strategically timing liposuction after GLP-1s like semaglutide or tirzepatide impacts safety, healing, and contours. Schedule surgery only after you’ve achieved a stable weight and metabolic status, as premature intervention can lead to suboptimal contouring and increased revisions. Aim for weight stabilization that endures for 3 to 6 months, as many surgeons like to see at least six months of steady weight prior to elective body-contouring surgery.
This lets soft tissues and skin adjust and provides a better sense of the remaining fat pockets that liposuction can tackle. Give your body time to acclimate to new weight and fat distribution. Fast loss alters skin laxity and the comparative size of fat deposits. Waiting allows skin to pull back where it can and defines where shaping is needed.
A patient who loses 12 kg in six months may see abdominal skin soften and internal fat shift. Waiting three to six more months often shows whether skin will tighten enough or if excision plus liposuction is required. If weight keeps dropping post-surgery, outcomes can become patchy.
Plan surgery when your weight loss has plateaued for optimal contouring. When weight stops coming off, it means metabolism is firm and the surgeon will know what the anatomy is like. For weekly GLP-1s with a half-life close to a week, specialists often suspend the medication one or more weeks prior to surgery to mitigate risks.
For certain drugs with slower clearance, it may even be safer to hold them for up to four weeks, as approximately half the drug clears each week. Just two missed days will not clear the stomach sufficiently for a safe procedure, and even after standard fasting periods, some gastric motility may persist which can compromise anesthesia risk.
Design a feasible schedule for moving from GLP-1 to surgery. Begin with a pre-op review three months before planned surgery to reconfirm stable weight for three to six months and to evaluate comorbidities. If recommended to discontinue the weekly GLP-1, schedule cessation one to four weeks pre-op depending on half-life and your surgeon’s recommendations.
Whenever possible, maintain stable weight six to twelve months post-therapy initiation at the time of elective surgery. This window fosters durable change and minimizes the likelihood of repeat surgery. Delay surgery if the weight is still changing or metabolic markers are still shifting.
Strategic timing involves coordinating decisions among the patient, the prescribing clinician, and the surgeon. Explicit discussions around medication half-life, fasting requirements, and weight stabilization timelines result in safer surgeries and more optimal results.
Holistic Contouring
Holistic contouring integrates GLP-1 meds with precise surgical and non-surgical therapies to sculpt form post-medical weight loss. It is a strategic schedule that works across several areas of the body, tackles loose skin and muscle depletion, and combines medical treatment with lifestyle and mental health assistance to achieve sustainable, realistic outcomes.
Lifestyle Foundation
Sustainable change requires steady habits that outlive drugs and surgery. Patients can pursue a high-protein diet and consistent strength training to minimize muscle wasting associated with GLP-1s and to enable recovery post-procedures.
Cardio, mobility work, and slow progressive resistance training preserve lean mass and maintain weight. Bad choices, such as neglecting strength work, depending on processed food, or abandoning activity, can erase drug and surgery gains and cause noticeable weight bounce back in treated and untreated zones.
Aim for lean mass-based protein targets, slow caloric nudges, and a lifestyle-compatible routine.
| Recommended Practices | Purpose |
|---|---|
| High-protein meals (1.2–2.0 g/kg body weight) | Preserve muscle, support recovery |
| STRENGTH training 2 to 4 times a week | Rebuild and preserve lean mass |
| Aerobic activity 150 minutes a week | Cardio, calorie balance |
| Sleep 7 to 9 hours nightly | Hormone balance, recovery |
| Follow up with clinician | Track medications, surgery readiness |
Mental Health
Quick body transformation can trigger surprising emotional responses. Patients can feel bereft, disconnected from their body, or harbor false expectations about contour and pace of transformation.
Watch for body dysmorphia and refer early to mental health providers when worried. Incorporate a mental health checklist into care: baseline screening, ongoing brief assessments, and access to counseling if needed.
Psychological support improves adherence to diet and exercise and helps patients set attainable goals that reduce regret or pursuit of repeated procedures.
Non-Surgical Options
Non-surgical tools span radiofrequency, focused ultrasound, cryolipolysis and injectable deoxycholic acid. For small, focal fat pockets or mild skin laxity, they can provide minor contouring with less downtime than liposuction.
While effectiveness falls short of surgical removal for larger volume changes, these methods fit patients desiring minimal recovery or incremental improvements. They can supplement lifestyle work or provide a stopgap for patients not ready for surgery.
- Pros of surgical (liposuction, excisional skin surgery): more dramatic, predictable volume and shape change, address large areas.
- Cons of surgical: longer recovery, anesthesia risks, need to stop some GLP-1s before surgery.
- Pros of non-surgical: less downtime, lower immediate risk, and repeatable.
- Cons of non-surgical: limited effect, often requires multiple sessions, less reliable for loose skin.
Risks and Recovery
Liposuction after ongoing GLP-1 use, like semaglutide (Ozempic), shifts risk and recovery. Surgeons and patients need to balance surgical complications, healing dynamics and the possibility that weight shifts alter results. Below are crisp, concrete specifics to structure the planning and process.
Surgical risks and medication interactions
Liposuction carries known risks such as seroma (fluid pockets), uneven contour, infection, bleeding, and blood clots. GLP-1 drugs can impact appetite, stomach emptying, and weight in ways that may alter tissue quality and nutritional status. Malnutrition or rapid weight changes can impede wound healing and increase susceptibility to infection.
Some surgeons require patients to discontinue specific drugs as early as one month before surgery to reduce bleeding and healing complications, all of which should be aligned with the prescribing clinician. Once you stop medications and old behaviors return, the weight can return and thus the surgery result can change or even need a revision.
Talk about clot risk, anesthesia interactions, and if lab work or a surgery delay until weight has been stable for three to six months is required to minimize complications.
Early recovery: first two weeks
Anticipate swelling, bruising, and pain that is most severe in the first 1 to 2 weeks. Sleep is critical. Compression garments moderate swelling and mold the tissues. Wear them as prescribed.
Drainage tubes can be used as well and can potentially increase seroma risk if not cared for appropriately. Watch wounds for redness, increased pain, fever, or drainage, which are signs of infection. Eat lots of protein to aid tissue repair and heed the team’s medication and dressing directives.
Small walks aid circulation, but don’t do any heavy lifting or strenuous exercises.
Mid recovery: weeks 3–6
Swelling and pain typically find themselves in this window. Patients typically return to light duty and desk work. There is a slow return to activity, but hold off on high-impact exercise until the surgeon gives the okay.
Contour irregularities can continue to show up as swelling moves around. Massage or lymphatic drainage, if advised, can alleviate any residual swelling and enhance contour.
Long term healing and practical checklist
Complete recovery and ultimate outcomes may require 3 to 12 months. Scars fade, but TLC, sun-block, and scar therapy help it proceed faster.
Create a recovery checklist: pre-op medical clearance, medication plan with prescribing doctor, nutrition plan high in protein, compression garments, wound-care supplies, follow-up appointments, activity milestones, and emergency signs to watch for.
Have pragmatic weight expectations in mind if you stop GLP-1 therapy.
Conclusion
Liposuction brings form once Ozempic brings down the scale. We notice many patients on semaglutide still struggle with stubborn pockets of fat on the flanks, belly, and thighs. Liposuction vacuums out those pockets and sculpts sharp lines. The best results come when your weight has been stagnant for at least three months and your skin is bouncing back beautifully. Great candidates are healthy, have realistic goals, and take photos to monitor progress. Plan on local swelling, bruises, and several weeks of limited activity. A board‑certified surgeon and expert team minimize risk and accelerate recovery.
Example: A person lost 12 kg on Ozempic, kept weight steady, then had targeted liposuction to smooth waist and inner thighs. It looked natural and fit their frame.
If you want a plan that fits your goals, consult with a board-certified surgeon and your prescribing clinician.
Frequently Asked Questions
What is the difference between continuing Ozempic and having liposuction to refine results?
Liposuction eliminates persistent fat in specific locations. Ozempic suppresses appetite and body fat systemically. Together, Ozempic aids general fat reduction and liposuction carves precise curves for a polished figure.
Who is an ideal candidate for liposuction after Ozempic?
Best candidates are adults who are at or near their goal weight with stable weight, good skin quality and reasonable expectations. This requires a consultation with a board-certified plastic surgeon and your prescribing clinician.
How long should I wait after stopping or starting Ozempic before getting liposuction?
Weight has been stable for at least 3 months. Talk timing with both your surgeon and prescribing doctor since Ozempic can influence healing and metabolic response.
Will liposuction replace the need for Ozempic or ongoing weight management?
No. Liposuction addresses localized fat but won’t address metabolic factors contributing to weight gain. Follow with medical oversight, diet, and exercise for long-term maintenance of results.
What are the main risks of combining Ozempic use and liposuction?
Complications consist of delayed wound healing, infection, contour irregularities, and varied metabolic response. Comprehensive clinical evaluation and meticulous operative planning minimize complication risks.
How long is recovery after liposuction, and does Ozempic affect it?
Standard healing is 1 to 2 weeks for light activity and 4 to 6 weeks for complete healing. Ozempic could impact energy and healing. Your surgeon will guide medication timing and wound care.
How can I maximize long-term results after liposuction and Ozempic?
With a healthy diet, exercise, and follow-up, be sure to keep your healthcare team updated on your weight and metabolic health to maintain contours and overall health.